The U.S. Preventive Services Task Force, in updating its breast cancer screening draft recommendations, once again is making waves. Just as in 2009, when it said that routine breast cancer screening for women under age 50 was not necessary, the task force is reiterating that sentiment — but saying it in a different way.
In the intervening years, that’s become a less controversial opinion, partially because of growing evidence that too much screening can lead to anxiety-ridden false-positive results, overdiagnosis and overtreatment. On Monday, the USPSTF released its updated recommendations, which look very similar to the recommendations released in 2009.
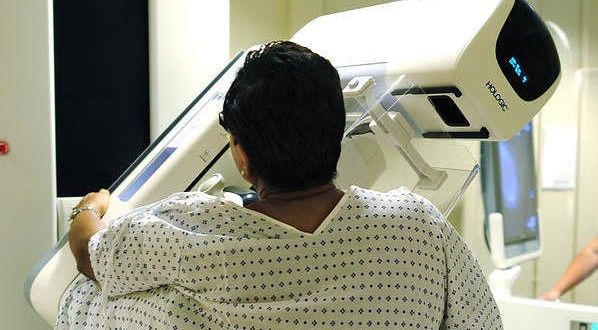
The new draft guidelines suggest women ages 50 to 74 get a mammogram every two years and women ages 40 to 49 should make their own decision on whether to start screening in consultation with their doctors. The task force also concluded that there was not enough evidence to make a recommendation for or against mammograms for women ages 75 and older, 3-D mammography or additional screening besides mammograms for women who have dense breasts. The guidelines will now undergo a public commenting period.
“In 2009, to suggest that mammography has limitations and that it has harms and that we need to look at the balance was not the way most people were thinking about it,” says Dr. Michael L. LeFevre, past chair of the USPSTF. “Much has been written about mammography in the last five years. I think people understand that it is a good test, it’s not a perfect test, and that there may be some significant harms associated with it.”
The task force added a nuance in the new guidelines that highlights which women might want to consider mammography more strongly, saying women in their 40s who have had a mother, sister or daughter with breast cancer are at a higher risk, and may benefit from mammography at a younger age than women who are at an average risk.
In the past year, there’s been compelling evidence in support of the 3-D mammogram as an accurate — and perhaps better — screening tool. One June study showed 3-D mammograms can pick up more breast cancers and lead to fewer callbacks for more testing than 2-D mammography. LeFevre says that while it’s a promising technology, he doesn’t think there is enough evidence to prove if it will result in improved health. “We are going to have to see more than just detection. There have to be more studies that look specifically at the outcomes in order for us to be certain,” he says.
Despite the fact that the mammogram recommendations happened over six years ago, many doctors still insist on yearly mammograms for their patients over age 40. The American Cancer Society also continues to recommend that women age 40 and up get yearly mammograms.
“There are plenty of women in the position with people just telling them you need to have a mammogram every year. I am somewhat embarrassed to admit that is still going on,” says LeFevre. “On the other hand, I think women are being more proactive about their discussions of mammography, and I think that’s reflective of the environment change we are in.”
The task-force guidelines are intended for women ages 40 and up who do not show signs of breast cancer, have never had breast cancer and do not have risk factors like a genetic mutation that put them at higher risk. High-risk patients should consult with their doctor for an individualized screening plan.
“Mammography helps. We can reduce women’s likelihood of dying of breast cancer by undergoing some regular screening at some interval during certain ages. That’s a common theme across almost all organizations that look at this,” says LeFevre. “We think we should be doing it in a way where we maximize the balance of benefits and harms. That’s our topline message and that’s what I hope women hear.”
Agencies/Canadajournal
 Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day
Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day


The American Cancer Society, a pawn group of the orthodox medical business, has been a crucial force to get mass mammography introduced by consistently downplaying and disregarding the known serious risks of the procedure while the group had consistently overstated its benefits.
No wonder Wender, a high official of the American Cancer Society, continues with the propaganda, claiming that “Mammography is the most effective way to reduce the likelihood of being diagnosed with advanced breast cancer, and avoiding a premature cancer death.”
There has never been much, if any, good evidence that mammography does anything of great significance in terms of breast cancer mortality reduction but (practically only medical industry-sponsored biased “studies” claim that), but plenty of sound data shows the test dose more serious harm than serious good (read ‘Mammography Screening: Truth, Lies and Controversy’ by Peter Gotzsche and ‘The Mammogram Myth’ by Rolf Hefti – see TheMammogramMyth dot com).
Most women are fooled by the misleading medical mantra that mammograms save lives simply because the public has been fed (“educated” or rather brainwashed) with a very one-sided biased pro-mammogram set of information circulated by the big business of mainstream medicine. Operating and reasoning based on this false body of information is the reason why very few women understand, for example, that a lot of breast cancer survivors are victims of harm instead of receivers of benefit. Therefore, almost all breast cancer “survivors” blindly repeat the official medical nonsense.
IF women (and men) at large were to scrutinize the mammogram data above and beyond the information of the mammogram industry (eg American Cancer Society, National Cancer Institute, Komen), they’d also find that it is almost exclusively the big profiteers of the test (eg radiologists, oncologists, medical trade associations, breast cancer “charities” etc) who promote the mass use of the test and that most pro-mammogram “research” is conducted by people with massive vested interests tied to the mammogram industry.
Luckily, more and more women and men have been waking up to the scam that it is.