Canadians with cystic fibrosis live 10 years longer on average than US patients, likely because of differences in the two countries’ health systems, researchers report in a study published online in the Annals of Internal Medicine.
After adjusting for differences among patients’ overall health, disease severity, and clinical factors, a team of American and Canadian scientists found that cystic fibrosis patients’ median age of survival is 50.9 years in Canada and 40.6 years in the US. Though the study did not fully assess the causes for the “significant survival gap,” the researchers noted that better access to lung transplants and healthcare in general appeared to play a role.
In fact, when comparing Canadian patients who have universal, government-provided health insurance with US patients who have private insurance, the researchers found no difference in the risk of death. But, US patients with continuous or intermittent Medicare or Medicaid or with no insurance at all had 36 to 77 percent higher risks of death than their Canadian counterparts.
“Although we cannot draw definitive causal inferences from these analyses, the observed differences raise the question of whether a disparity exists in access to therapeutic approaches or health care delivery such that hypotheses may be generated for further investigation,” the authors conclude.
And further investigations are indeed warranted, researchers say. “A ten-year difference… that’s lots of years spent with your child or not, having fun with your friends, living your life,” epidemiologist Kevin Gorey of the University of Windsor, who was not involved with the study, told STAT. “That’s a huge, huge human tragedy.”
Previous estimates and assessments have pegged the survival rate of cystic fibrosis patients in developing countries from 41.5 to 50 years. But directly comparing survival data between countries is tricky because they may have different methods for tracking and recording patient health data.
To get around this, the authors of the new study tracked detailed health records of 5,941 Canadian patients across 42 cystic fibrosis care centers and 45,448 US patients across 110 care centers from 1990 to 2013. They also broke the patients into subgroups based on disease severity.
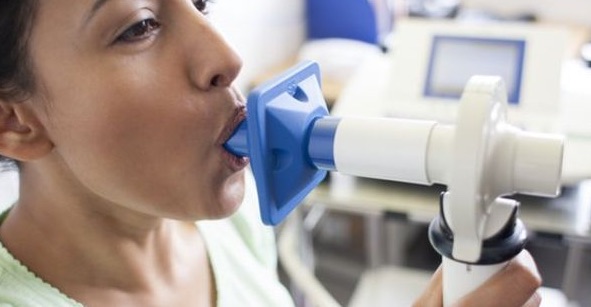
Cystic fibrosis is caused by a genetic mutation that breaks an ion channel in tissue-lining cells. The channel is necessary to properly make sweat, mucus, and digestive juices. Results of the mutation include thick mucus in the respiratory tract that can create a haven for deadly pathogens, as well as gastrointestinal issues and pancreas damage. The type of mutation, type of pathogens that settle in the lungs, pancreatic status, quality of care, and diet can all affect health outcomes.
But taking all of those factors into account and breaking patients up into severity subgroups, the researchers still found a big gap between US and Canadian patients’ survival. “The fact that our findings were consistent across several subgroups, including those with a severe clinical phenotype, suggests that longer survival in Canada than the United States is not the result of following patients with milder disease in the Canadian cohort,” the authors conclude.
The results fit with larger trends for the US, which has repeatedly ranked low relative to other developed countries when it comes to healthcare quality. In 2000, the World Health Organization ranked America’s health system 37 of 191 countries, just below Costa Rica. In 2014, private foundation the Commonwealth Fund ranked the US health system last among 11 wealthy countries. Currently, Americans’ life expectancy is among the lowest of wealthy countries and is projected to see the fewest gains in upcoming years compared with peers. The US also has the highest maternal and child mortality rates of wealthy countries.
Agencies/Canadajournal
 Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day
Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day