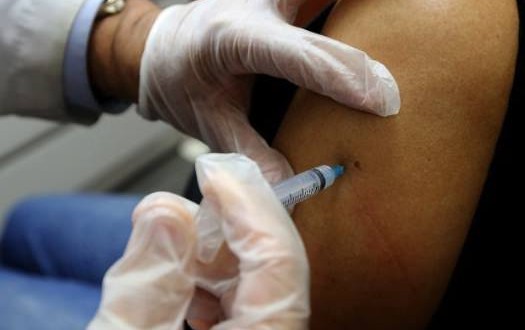
Millions of American adults are failing to get vaccinated against whooping cough, tetanus, shingles and other diseases, the CDC said Thursday.
New immunization rates released this week fall far short of national goals for recommended vaccines, according to the U.S. Centers for Disease Control and Prevention data.
Just 14 percent of adults 19 and older are vaccinated against tetanus, diphtheria and whooping cough. Only 20 percent age 60 and older received the shingles vaccination, and only about 35 percent of women ages 19 to 26 are immunized against HPV, or human papillomavirus.
Press Releases
Low vaccination rates leave millions of Americans vulnerable to preventable diseases and are a driver of avoidable healthcare costs. Gaps in immunizations are also contributing to the resurgence of illnesses, like whooping cough. Immunizing adults not only protects the individual but helps avoid spreading the disease to children and other adults.
In 2012, there were more than 48,000 cases of whooping cough in the United States – the highest incidence reported since 1955 – according to the CDC. Treating whooping cough is far more costly than taking preventive action, with treatment costs around $2,000 per case, compared to a few dollars per dose of vaccine.
In December, Trust for America’s Health (TFAH) and the Robert Wood Johnson Foundation (RWJF) issued the Outbreaks: Protecting Americans from Infectious Diseases report, which identified several reasons why immunization rates remain low, including:
Misunderstanding and misinformation: Many Americans do not understand the safety and effectiveness of vaccines, including the rigorous approval and safety processes put into place by the Food and Drug Administration (FDA);
Limited access: Currently, there is no real system or structure in place to ensure that most adults receive the vaccinations they need. Many adults do not have regular well care exams, switch doctors or health plans often, do not have ready access to their past medical histories or only seek care from specialists who do not traditionally screen for immunization histories or offer vaccines.
Limited data sharing: The country’s immunization registry system is underfunded and underutilized, which makes it difficult to track whether adults are up-to-date with recommended vaccinations. Vaccines must be integrated into electronic health records to give patients and their doctors the ability to track immunization status in an effective and efficient way; and
Limited care and insurance coverage: While the Affordable Care Act (ACA) now requires no cost sharing for in-network providers for recommended vaccinations for adults enrolled in group and individuals plans or who are part of Medicaid expansion, most adults do not know when to request vaccinations and their past histories are often not tracked by doctors. In addition, co-pay requirements for the base Medicaid population varies by state and Medicare does not consistently provide first dollar coverage for vaccines.
“Some of the greatest public health successes of the past century — including the worldwide eradication of smallpox and the virtual elimination of polio, measles and rubella in the United States — are because of successful vaccination programs,” said Jeffrey Levi, PhD, executive director of TFAH. “We know that vaccines are safe and save lives. Yet millions do not get routine immunizations and tens of thousands die each year as a result.”
“The current rates are truly abysmal and we need to radically rethink how we can increase rates. Strategies that can make a difference include ensuring adults actually receive expanded preventive services covered under the ACA, growing the use of electronic health records to track when adults are due for recommended shots, and improving coverage for all Medicare and Medicaid beneficiaries,” Levi continued.
Some recommendations highlighted in the Outbreaks report that could improve adult immunization rates include:
Increasing public education about the importance of getting vaccinated – and the safety of vaccines;
Expanding support for immunization programs, making it easier and more convenient to get vaccinated;
Ensuring first dollar coverage of all recommended vaccines under Medicare;
Facilitating the expansion of settings where vaccinations can be given and can receive adequate reimbursement;
Improving and modernizing surveillance and diagnostics; and
Funding and incentivizing vaccine research.
Canadajournal/Press Releases
 Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day
Canada Journal – News of the World Articles and videos to bring you the biggest Canadian news stories from across the country every day